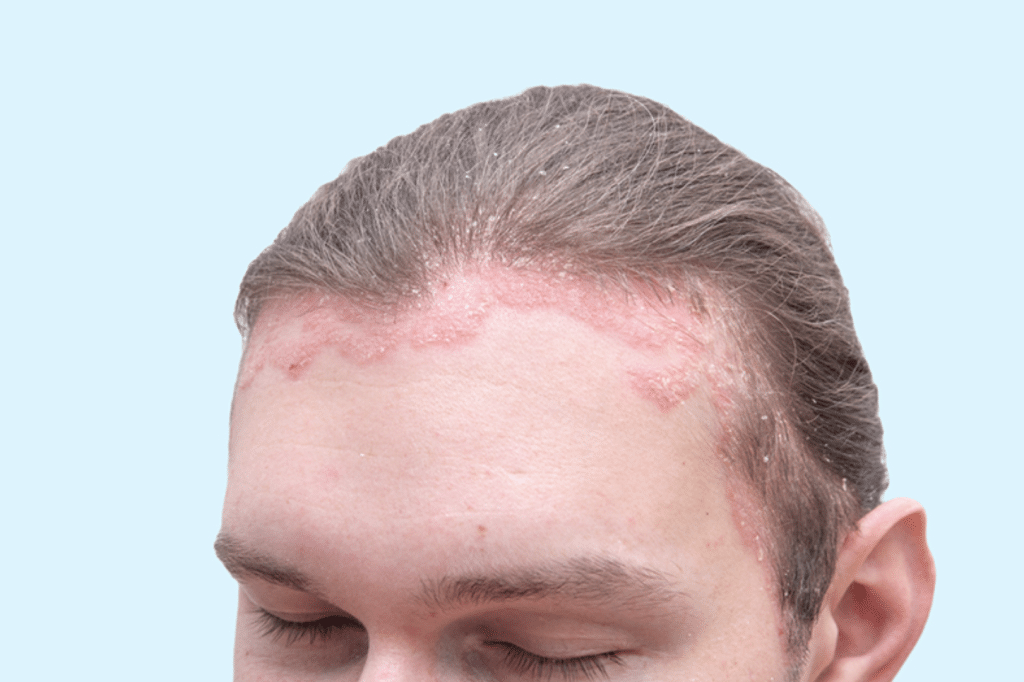
Psoriasis is a chronic autoimmune disorder that affects the skin. It causes rapid buildup of skin cells, resulting in thick, red, and scaly patches on the skin. These patches can be itchy, painful, and can occur anywhere on the body, but are commonly found on the scalp, elbows, knees, and lower back.
While there is no cure for psoriasis, several treatment options are available to manage the symptoms and reduce the frequency and severity of flare-ups. The choice of treatment depends on the type and severity of psoriasis, as well as individual factors such as overall health and personal preferences. Here are some common treatment approaches on how to treat psoriasis:
Topical Treatments: These are applied directly to the skin and are typically the first line of treatment for mild to moderate psoriasis. They include corticosteroids, vitamin D analogs, retinoids, coal tar, salicylic acid, and moisturizers. These medications help to reduce inflammation, slow down the growth of skin cells, and alleviate itching and scaling.
Phototherapy: This involves exposing the affected skin to specific wavelengths of ultraviolet (UV) light under medical supervision. Phototherapy can be done using artificial light sources (UVB lamps) or natural sunlight (controlled exposure). The light helps to slow down the growth of skin cells and reduce inflammation.
Systemic Medications: These are prescribed for moderate to severe psoriasis or when other treatments have not been effective. Systemic medications are taken orally or by injection and work throughout the body. They include methotrexate, cyclosporine, acitretin, and newer biologic drugs such as TNF-alpha inhibitors, interleukin inhibitors, and phosphodiesterase-4 inhibitors. These medications target specific aspects of the immune system to reduce inflammation and control the overactive immune response.
Oral Retinoids: Retinoids are derived from vitamin A and are used for severe cases of psoriasis that do not respond to other treatments. Oral retinoids work by suppressing the immune system and reducing inflammation. However, they may have significant side effects and are generally used for short periods.
Injectable Biologics: Biologic drugs are derived from living sources and target specific parts of the immune system involved in psoriasis. They are administered by injection or infusion and are highly effective for severe psoriasis.
It’s important to note that treatment plans may vary from person to person, and it’s best to consult a holistic dermatologist or healthcare professional to determine the most suitable treatment approach based on individual circumstances and needs.
Psoriasis is a chronic skin condition that causes red, itchy, and scaly patches on the skin. While there is no cure for psoriasis, there are several natural remedies and lifestyle changes that may help manage its symptoms. It’s important to note that natural remedies may not work for everyone, and it’s always a good idea to consult with a healthcare professional for proper diagnosis and advice concerning how to treat psoriasis. Here are some natural approaches that you can consider:
1. Moisturize:
Keeping your skin well-moisturized can help reduce itching and dryness. Use a gentle, fragrance-free moisturizer or natural oils like coconut oil, olive oil, or almond oil after bathing.
2. Avoid triggers:
Identify and avoid triggers that worsen your psoriasis symptoms. Common triggers include stress, certain foods, alcohol, smoking, and cold weather. By minimizing exposure to these triggers, you may be able to reduce flare-ups.
3. Warm baths:
Soaking in a warm bath with added oatmeal, Dead Sea salts, or Epsom salts can help soothe the skin and relieve itching. Make sure the water is not too hot, as hot water can worsen psoriasis symptoms.
4. Sunlight exposure:
Limited exposure to sunlight can improve psoriasis symptoms for some individuals. However, it’s essential to balance sunlight exposure to avoid sunburn. Start with short periods of sun exposure and gradually increase the duration. Use sunscreen on unaffected areas.
5. Diet and nutrition:
While there is no specific psoriasis diet, maintaining a healthy diet may support overall skin health. Include plenty of fruits, vegetables, whole grains, lean proteins, and omega-3 fatty acids from sources like fatty fish or flaxseeds. Avoid or limit processed foods, sugary snacks, and alcohol, as they may trigger inflammation.
6. Stress management:
Stress can exacerbate psoriasis symptoms for many people. Engage in stress-reducing activities like exercise, meditation, yoga, deep breathing exercises, or hobbies you enjoy to help manage stress levels.
Natural topical treatments:
Certain natural substances may provide relief when applied topically. These include aloe vera gel, tea tree oil, apple cider vinegar (diluted with water), and capsaicin cream (derived from chili peppers). However, it’s important to patch test these remedies on a small area of skin first and discontinue use if any irritation occurs.
Remember, these natural remedies may not work for everyone, and their effectiveness can vary. It’s crucial to consult with a holistic dermatologist or healthcare professional for a proper diagnosis and personalized treatment plan for your specific condition. They can provide guidance and recommend appropriate treatment options based on the severity of your psoriasis.